- AdventHealth University
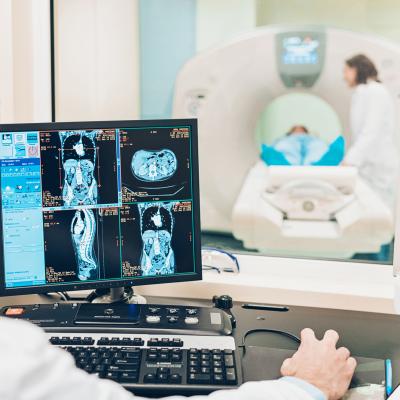
By 2050, 16% of the world’s population will be older than 65 according to United Nations population estimates, which points to a rising need for safer, more efficient, and less expensive medical procedures. Thankfully, advances in imaging technologies allow healthcare providers to diagnose vascular conditions and perform minimally invasive procedures such as stenting, angioplasty, and biopsy more easily.
Vascular interventional radiology is the practice of using a combination of catheter-based procedures and imaging technology, such as ultrasound and digital X-ray, to diagnose and treat disease. It focuses on blood vessels and the lymphatic system and can be used to treat a wide range of conditions — from cancer to infertility.
The many benefits of interventional radiology for patients include less pain, lower risk, and shorter recovery time compared with traditional surgery. Medical imaging professionals interested in advancing their careers in the field should consider pursuing an Advanced Imaging Certificate in Vascular Interventional Radiography, which can help them pursue a career as an interventional technologist. Interventional technologists assist physicians in conducting interventional radiology procedures.
How Vascular Interventional Radiology Works
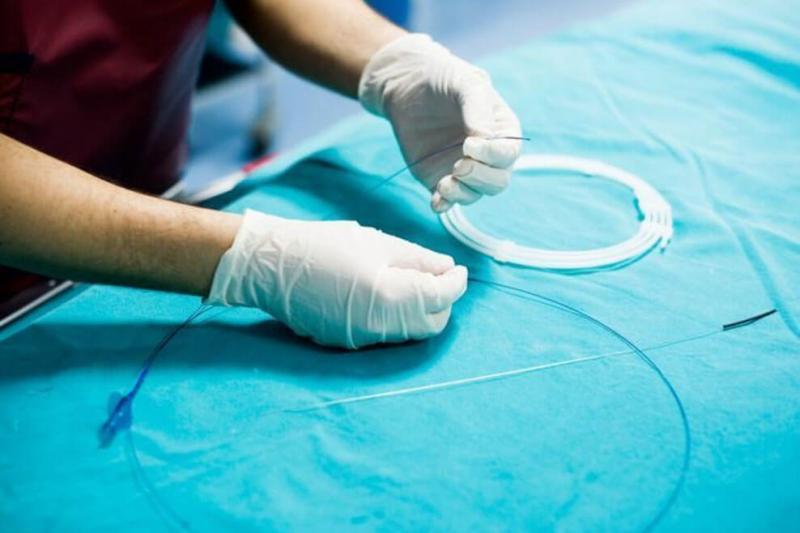
In 1953, Swedish radiologist Sven-Ivar Seldinger developed a technique to use a flexible wire to guide a catheter to different parts of the body. According to the eponymous Seldinger technique, a medical professional punctures a vessel or cavity with a sharp hollow needle, using ultrasound as guidance if necessary.
Then, the medical professional pushes a guidewire through the needle into the body, enabling them to remove the needle and pass a sheath or tube into the area. This final step allows professionals to insert catheters or other devices, which they can then navigate all over the body from the small incision.
Through an opening that is only a few millimeters wide, vascular interventional radiologists — with the assistance of vascular interventional technologists — can treat a wide range of conditions.
Sometimes called “surgery without a knife,” vascular interventional radiology uses ultrasound, computed tomography (CT), MRI, or real-time X-rays — or, at times, a combination of imaging technologies — to guide equipment to access internal organs and structures.
To navigate a vessel, professionals with this training may perform fluoroscopy, the practice of using equipment to project a continuous X-ray beam through the body to an examination site in real time. Vascular interventional professionals closely watch the images resulting from the x-ray beam transmission on a digital monitor to view bodily structures and movement in detail.
Veins and arteries have no nerves, so patients undergoing these procedures typically do not need general anesthesia and experience only mild to moderate post-procedure pain. Most vascular interventional radiology procedures are performed on an outpatient basis, allowing patients to return home the same day without a lengthy hospital stay. This small incision site can heal quickly and easily after a procedure — one of the many benefits of interventional radiology.
Applications of Interventional Radiology
The applications of interventional radiology are many. From a single incision, interventional technologists and radiologists can work together to:
- Use fluoroscopy to maneuver a catheter to previously unreachable parts of the body (e.g., to treat internal bleeding in the arteries that supply the kidneys)
- Inject contrast media to visualize vessels and organs (e.g., to locate and treat uterine fibroids)
- Insert a drainage tube into a bile duct in the liver to remove blockage and allow bile to flow into the small intestine (biliary drainage)
- Unblock blood vessels and arteries (angioplasty) to restore blood flow (e.g., to treat a narrowed carotid artery using a balloon and stent to restore blood flow to the brain)
- Conduct state-of-the-art local tumor cell destruction procedures such as thermoablation (using high temperatures and electroporation to eliminate tumors)
Interventional technologists contribute to medical care teams in fields including gastroenterology, gynecology, oncology, cardiology, and urology.
Case Study in Vascular Interventional Radiology: Embolization in Oncology
Tumors require a constant blood supply to grow. By cutting off their blood supply, harmful tumors will shrink and eventually die. Embolization is a procedure performed by interventional radiology teams to do just that.
During an embolization, patients commonly encounter the following procedures:
- Before the procedure, patients are typically instructed to not eat anything and may be given a sedative to help them relax. Keeping patients calm during the procedure ensures that the X-ray images accurately reflect the bodily structures inside.
- The interventional technologist will help position the patient and select the appropriate settings on the imaging equipment settings.
- In a procedure that can last less than an hour, the interventional radiology team may start by providing some local anesthetic and then making a tiny puncture in an artery (usually located in the wrist, thigh, or groin) with a small needle.
- Interventional radiologists can then thread a combination of guidewires and plastic tubes (sheaths and catheters) into the patient’s arteries, with positioning and imaging guidance from the interventional technologist.
- By injecting a contrast medium, the professionals can see an area of the body more clearly under imaging.
- With a clear view, the radiologist can carefully navigate a microcatheter to a tumor and release embolic particles to cut off blood flow to the tumor and impede its growth.
- In cancer treatments, embolic particles may be combined with chemotherapy.
While patients sometimes experience some mild pain and nausea post procedure, they’re most often able to return home the same day. Care professionals then follow up with patients to make sure that their pain is manageable and normal (often with painkillers and nausea preventive medicine) and they recover quickly.
How Interventional Radiology Benefits Patients and Professionals
Interventional radiology offers a host of benefits compared with traditional open surgery. For example, according to the University Diagnostic Medical Imaging (UDMI), open surgery typically involves more blood loss and a higher risk for infection and other complications than interventional radiology.
Greater Efficiency
Radiologists and technologists have high visibility when using medical imaging technology during vascular procedures. Throughout the procedure, professionals can accurately diagnose and treat conditions, sometimes in less than an hour.
Because these procedures are relatively quick, they’re also considered a more efficient use of medical resources than full surgery. Most outpatient procedures, including interventional radiology, are less expensive than inpatient hospital stays, so interventional radiology is often a more cost-effective procedure for patients.
Faster Recovery
Another one of the many benefits of interventional radiology is an often swift, uncomplicated recovery. A shorter recovery time means that patients can return to their daily activities faster.
Due to the minimally invasive nature of interventional radiology procedures, patients can return home afterward and may fully recover within days rather than weeks.
Better Outcomes
The rapidly evolving specialty of interventional radiology has a low complication rate and low mortality rate as a result of its minimal invasiveness. Interventional radiology can be used to treat almost anybody: young or old, large or small. Therefore, interventional radiology is well received by patients who enjoy a fast, safe route to health.
Advance Your Career in Interventional Radiology
If you have an associate degree in radiography and are ARRT certified, consider taking the next step in your career by earning the Advanced Imaging Certificate in Vascular Interventional Radiography from AdventHealth University Online and becoming a vascular interventional technologist.
The program is designed for professionals who want to go to school while working full time. Take charge of your career and learn more about how earning an advanced certificate can be the first step toward a Bachelor of Science in Imaging Sciences.
Recommended Readings:
What Is Vascular Interventional Radiology?
MRA vs. MRI: What Are the Differences and Uses?
Sources:
Advantage IR, “Top 5 Reasons Why Interventional Radiology Is Better Than Open Surgery”
American Registry of Radiologic Technologists (ARRT), Postprimary Eligibility Pathway Requirements
American Registry of Radiologic Technologists (ARRT), Vascular Interventional Radiography
Radiological Society of North America, “Value in Interventional Radiology: Achieving High Quality Outcomes at a Lower Cost”
Society of Interventional Radiology, Frequently Asked Questions
University Diagnostic Medical Imaging, Advantages and Benefits of Interventional Radiology (IR)
United Nations, Global Issues: Ageing